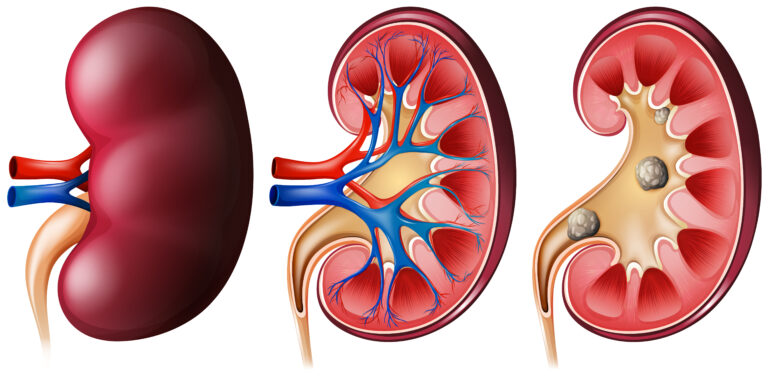
Kidney stones are hard deposits made of minerals and salts that form inside your kidneys. They can range in size from a grain of sand to a golf ball. While small stones may pass unnoticed, larger ones can cause significant pain and complications.
Here’s a breakdown of common aspects related to kidney stones:
Symptoms:
The pain associated with kidney stones, often called renal colic, is often described as one of the most severe types of pain. Symptoms can include:
Severe pain: This pain typically starts suddenly and can be felt in your back, side, lower abdomen, or groin. It often comes and goes in waves and changes location and intensity as the stone moves.
Pain or burning during urination: This can occur when the stone reaches the junction between your ureter and bladder.
Frequent or urgent need to urinate: You may feel the need to urinate more often or with greater urgency than usual.
Blood in the urine (hematuria): Your urine may appear pink, red, or brown. Sometimes, the blood cells are too small to see without a microscope.
Cloudy or foul-smelling urine: This can be a sign of infection.
Nausea and vomiting: These symptoms are common due to shared nerve connections between the kidneys and the gastrointestinal tract.
Fever and chills: These are serious signs that could indicate an infection in your kidney or urinary tract and require immediate medical attention.
Urination of small amounts or inability to urinate: A large stone can block the flow of urine, leading to this. Complete blockage is a medical emergency.
Causes:
Kidney stones form when there’s an imbalance of certain substances in your urine, leading to crystal formation. Common causes and risk factors include:
Dehydration: Not drinking enough fluids is a major risk factor, as it leads to more concentrated urine where minerals can easily crystallize.
Diet:
High salt intake: Can increase calcium levels in your urine.
High animal protein diet: Can increase uric acid levels.
Low calcium intake: Can paradoxically increase the risk of calcium oxalate stones because calcium helps bind oxalate in the gut, preventing it from reaching the kidneys.
High oxalate foods: Oxalate is a natural substance found in many foods (e.g., spinach, beets, almonds, soy products).
Excessive sugar or carbonated soft drink consumption.
Medical conditions:
Urinary tract infections (UTIs) can lead to struvite stones.
Certain metabolic disorders (e.g., gout, which causes high uric acid levels).
Hyperparathyroidism (overactive parathyroid glands leading to high calcium levels).
Some inherited conditions (e.g., cystinuria).
Obesity and diabetes.
Medications: Certain medications like aspirin, antacids, diuretics, some antibiotics, and antiretroviral medicines can increase the risk.
Family history: A family history of kidney stones increases your likelihood of developing them.
Previous kidney stones: If you’ve had a kidney stone before, you’re more likely to have another.
Lack of physical activity or prolonged bed rest.
Treatment:
Treatment depends on the size, type, and location of the stone, as well as the severity of symptoms.
For small stones (often less than 6mm) with mild symptoms:
Drinking plenty of fluids: Especially water, to help flush the stone out. Aim for clear or nearly clear urine.
Pain relievers: Over-the-counter medications like ibuprofen or naproxen, or stronger prescription pain medications.
Alpha-blockers: Medications like tamsulosin (Flomax) can relax the muscles in your ureter, making it easier to pass the stone.
Anti-sickness medicine: To manage nausea and vomiting.
For larger stones or those causing severe symptoms/complications:
Extracorporeal Shock Wave Lithotripsy (ESWL): Uses sound waves to break the stone into smaller pieces that can be passed in urine. This is a non-invasive procedure.
Ureteroscopy: A thin, lighted tube (ureteroscope) is inserted through the urethra and bladder into the ureter to locate the stone. The surgeon can then remove the stone with a basket-like tool or break it up with a laser. A stent may be placed to aid healing and urine flow.
Percutaneous Nephrolithotomy (PCNL): For very large stones, a small incision is made in your back, and a thin telescope (nephroscope) is inserted directly into the kidney to remove the stone or break it into smaller pieces. This usually requires a hospital stay.
Open surgery: Rarely performed nowadays due to advancements in minimally invasive techniques, but may be necessary for very complex cases.
Medications to prevent future stones: Depending on the stone type, medications like potassium citrate, allopurinol, or antibiotics may be prescribed.
Surgery for hyperparathyroidism: If the stones are caused by an overactive parathyroid gland, surgery to remove the affected gland can prevent future stone formation.
Prevention:
The best ways to prevent kidney stones include:
Staying well-hydrated: Drink plenty of water throughout the day to keep your urine diluted.
Dietary modifications:
Limit salt intake.
Reduce animal protein consumption.
Ensure adequate calcium intake from food (not supplements, unless advised by a doctor).
Limit high-oxalate foods if you are prone to calcium oxalate stones, but don’t eliminate them entirely without professional advice.
Avoid excessive consumption of sugary drinks.
Managing underlying medical conditions: Treat conditions like UTIs, gout, or hyperparathyroidism.
Medications: If you have recurrent stones, your doctor may prescribe medications to help prevent new ones.
If you suspect you have kidney stones, it’s crucial to seek medical attention promptly, especially if you experience severe pain, fever, chills, or blood in your urine.
